Is Connection the Cure? – News from Psychedelic Science 2017

There is increasing evidence that psychedelic-assisted psychotherapy can provide something that conventional antidepressants and talking therapies cannot. Over the last few years, small numbers of patients suffering from treatment-resistant depression and chronic anxiety disorders have been given psychedelics (psilocybin, LSD, ayahuasca, ketamine or MDMA) in combination with psychotherapy in clinical trials.
The results have been nothing short of remarkable. So much so, that in the US, the FDA have recently approved phase 3 studies of MDMA for post-traumatic stress disorder, and phase 3 psilocybin studies are not far behind. Phase 3 is the final stage of the drug approval process, which if successful, leads to the drug becoming a prescription medication.
Researchers, mental health professionals and participants involved in these pioneering trials recently gathered at the world’s largest psychedelic conference, Psychedelic Science 2017, co-hosted by the Beckley Foundation and MAPS. Sharing their results and experiences, study after study revealed a high percentage (40-80%) of participants being symptom free at the end of the trials. What’s more, the positive effects endure for several months, and in some cases years. These outcomes occurred with as few as one or two sessions of psychedelic-assisted psychotherapy, instead of the usual long courses of talking therapies, or daily dependency on antidepressant medications that can have unpleasant side effects.
Precisely how the psychedelic experience has such profound and long-lasting therapeutic effects was explored at great depth by scientists and thinkers from a wide variety of disciplines. A central theme that emerged was that of connection: the ability of psychedelics to create new connections or facilitate reconnection. A feeling of disconnection is a common feature of mental health disorders. This includes disconnection from the world, disconnection from others, and disconnection from self. Gabor Maté, a keynote speaker at Psychedelic Science, discussed how childhood trauma can cause this. Unable to bear the pain/self loathing/shame etc that arises from trauma, the individual disconnects from themselves as a survival strategy. “Depression” he says, “means to push something down…..namely the emotions”. Modern medicine doesn’t attempt to reach these repressed emotions or disconnected parts of the self, but rather pathologizes the presenting symptoms and targets the condition with pharmaceutical drugs.
A feeling of disconnection is a common feature of mental health disorders. This includes disconnection from the world, disconnection from others, and disconnection from self. Gabor Maté, a keynote speaker at Psychedelic Science, discussed how childhood trauma can cause this. Unable to bear the pain/self loathing/shame etc that arises from trauma, the individual disconnects from themselves as a survival strategy. “Depression” he says, “means to push something down…..namely the emotions”. Modern medicine doesn’t attempt to reach these repressed emotions or disconnected parts of the self, but rather pathologizes the presenting symptoms and targets the condition with pharmaceutical drugs.
Carefully controlled psychedelic experiences, on the other hand, enable people to explore the underlying causes of their suffering, to reconnect with the injured self, and to re-integrate painful and repressed memories. This can facilitate increased self-acceptance, which then in turn promotes connections to others.
Dr Ros Watts (Beckley/Imperial Psilocybin for Depression Study) and Mary Cosimano (Johns Hopkins Psilocybin Studies) further supported this idea by sharing their observations in the trials, and recounting the experiences of numerous participants, who had been helped to connect with self, friends, family, the wider community and spirit.
Mary quoted a participant from the Johns Hopkins psilocybin study;
“My single strongest memory will be from the first session when I found myself chasing something that had been eluding me. When I caught it, I discovered that it was me. The subsequent rejoining seems to me to be the single most powerful event in my life. I feel whole for the first time and able to cope with anything. Apart, I was weak and directionless. Listless, really. But together, I am strong, capable of anything and just happier.”
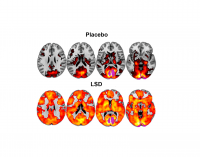
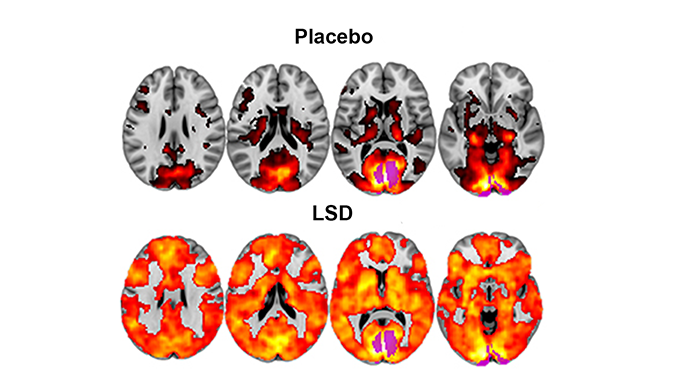
Connections are also taking place within the brain, as demonstrated by the Beckley/Imperial Research Programme’s brain-imaging studies. Images show that psilocybin and LSD cause increased connectivity between brain regions that don’t usually communicate, leading to a more integrated whole brain.
The spiritual significance of the psychedelic experience was also something that was highlighted throughout the conference. From the Beckley/Imperial psilocybin research team, Leor Roseman explained how higher ratings of feelings of unity, spiritual experience, blissful state and insightfulness, all correlated with higher reductions in depressive symptoms. In the Johns Hopkins, Psilocybin for Smoking Cessation study, 60% of participants met the criteria for complete ‘mystical experience’, and smoking cessation outcomes were strongly correlated with this.
Amanda Fielding reported that, “Our research is repeatedly confirming what we had expected – that psychedelics can evoke powerful, often transcendent experiences, that can lead to positive changes in mood, well-being and personality traits, persisting for days, weeks or even years”.
In an era in which mental health disorders are reaching epidemic proportions, with 1 in 4 people globally experiencing a mental illness at some point in their lives, and 1 in 3 teenage girls in the UK suffering from depression or anxiety, contemporary psychiatry needs to find a way to address the underlying causes of mental health dysfunction, and expand the pharmacopeia to include substances that have the potential to cure these conditions, rather than simply treat them.
Stripped of the political baggage that psychedelics have accumulated over the years, there is growing consensus that they hold considerable potential for mental healthcare, and indeed for creating a shift in the way we view mental health and its treatment. Although psychedelic research is still in its infancy, we are gradually gaining a better understanding of how these compounds produce such enduring positive effects. The take-home message was that increased connectivity may pave the road away from addiction, depression and anxiety disorders, towards improved well-being and a healthier society.
Words: Hattie Wells
Podcast
- All
Links
- All
Support
- All
BIPRP
- All
Science Talk
- All
Amanda's Talks
- All
- Video Talk
- Featured
- 2016 Onwards
- 2011-2015
- 2010 and Earlier
- Science Talk
- Policy Talk
One-pager
- All
Music
- All
Amanda Feilding
- All
Events
- All
Highlights
- All
Psilocybin for Depression
- All
Current
- All
Category
- All
- Science
- Policy
- Culture
Substance/Method
- All
- Opiates
- Novel Psychoactive Substances
- Meditation
- Trepanation
- LSD
- Psilocybin
- Cannabis/cannabinoids
- Ayahuasca/DMT
- Coca/Cocaine
- MDMA
Collaboration
- All
- Beckley/Brazil Research Programme
- Beckley/Maastricht Research Programme
- Exeter University
- ICEERS
- Beckley/Sant Pau Research Programme
- University College London
- New York University
- Cardiff University
- Madrid Computense University
- Ethnobotanicals Research Programme
- Freiburg University
- Medical Office for Psychiatry and Psychotherapy, Solothurn
- Beckley/Sechenov Institute Research programme
- Hannover Medical School
- Beckley/Imperial Research Programme
- King's College London
- Johns Hopkins University
Clinical Application
- All
- Depression
- Addictions
- Anxiety
- Psychosis
- PTSD
- Cancer
- Cluster Headaches
Policy Focus
- All
- Policy Reports
- Advisory Work
- Seminar Series
- Advocacy/Campaigns
Type of publication
- All
- Original research
- Report
- Review
- Opinion/Correspondence
- Book
- Book chapter
- Conference abstract
- Petition/campaign
Search type